How Early Access Signal Detection Protects Your TRx in a Changing Payer Landscape

In late 2024, market access teams responsible for Part B infused therapies began noticing the same unsettling pattern. Hospital outpatient departments were administering fewer infusions. Prescribers were still writing orders, but patients were increasingly being routed to physician offices and standalone infusion centers.
CMS had not yet finalized the next expansion of site-neutral payment. Claims data still looked stable, and quarterly reports showed no obvious drop in total prescriptions. Yet field teams were hearing it directly from providers and IDNs. Payers were already signaling preferred sites of care. Network steerage was happening quietly, well before reimbursement rules caught up.
Oncology was simply the first area where these dynamics became visible at scale, before spreading across other infused and administered therapies.
By the time CMS advanced site-neutral payment under the CY 2026 Hospital Outpatient Prospective Payment System, the volume shift was no longer a hypothesis your team was monitoring. It was a completed migration, and you were now managing the aftermath.
This is the new rhythm of access risk in market access in healthcare. It does not arrive as a single policy shock that triggers immediate response. Instead, it develops upstream, through changes in benefit design and network steerage that rarely make headlines. By the time retrospective actuarial analytics confirm the pattern, you have already lost 90 days of opportunity to protect TRx and adjust your market access strategy.
How Humbi’s Actuarial Intelligence Delivers Early Access Signal Detection
Most market access teams don’t suffer from a lack of data. They suffer from timing. By the time claims confirm that access has tightened, the opportunity to intervene has already passed.
Humbi by Innovaccer was built to change when access risk becomes visible.
When your team opens Humbi, the starting point is a current-state view of how TRx is flowing today, across payers and sites of care, grounded in continuously refreshed claims data.
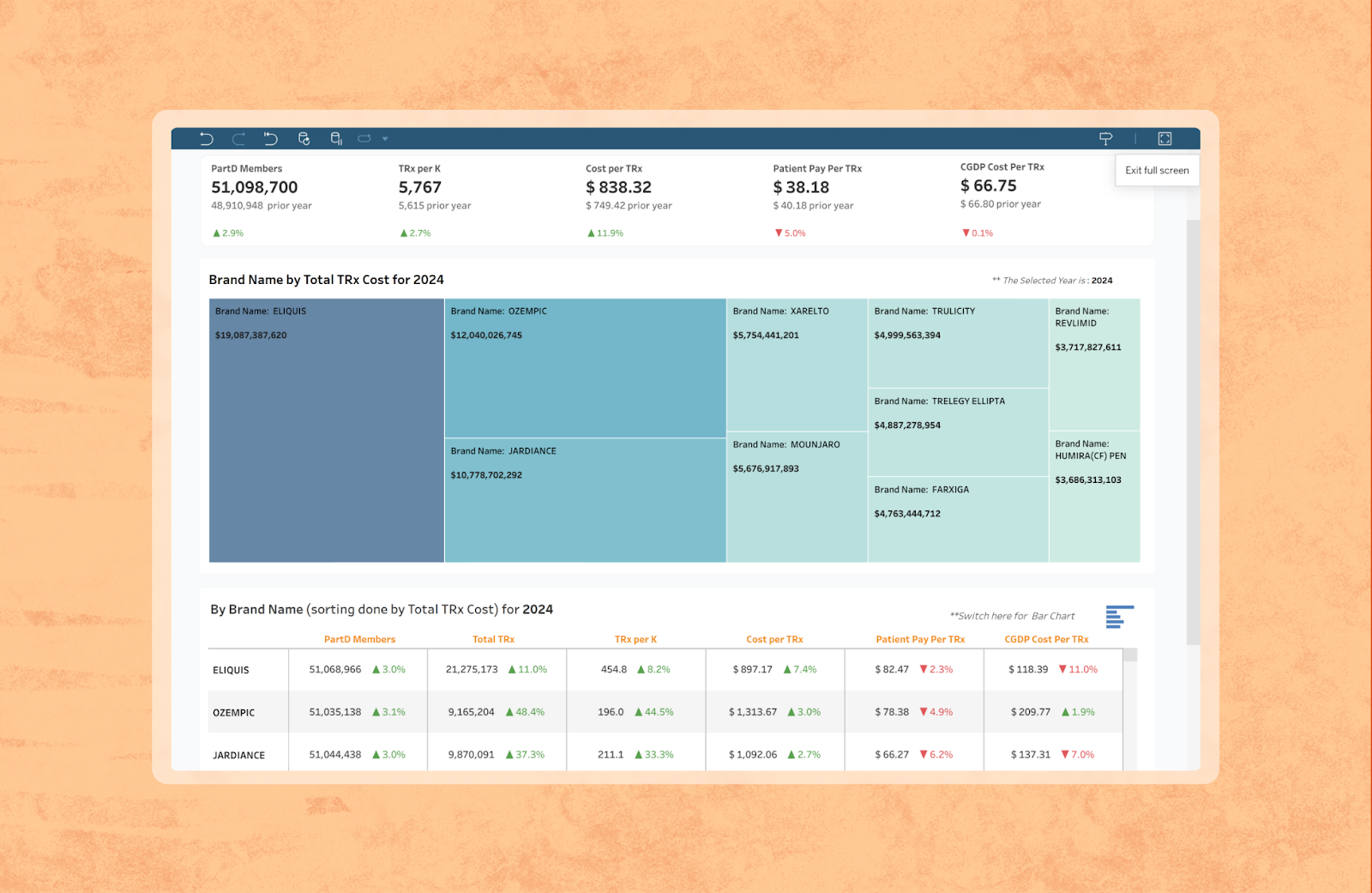
You can immediately see where therapies are being administered, how volume is distributed across Medicare, Medicaid, and commercial payers, and which care settings are driving utilization. That baseline matters, because early access detection only works if you understand what “normal” looks like for each product and channel.
Humbi establishes that baseline using monthly, claim-line level updates across Medicare fee-for-service, Medicare Advantage, Medicaid (T-MSIS), and commercial populations, covering approximately 150M+ covered lives depending on channel and year.
Seeing Access Risk While It Is Still Forming
Once the baseline is set, Humbi begins surfacing the signals that historically precede TRx disruption. In practice, this happens through a combination of payer landscape dashboards, policy impact monitoring, site-of-care utilization views, and configurable business rules that flag deviation from historical access patterns. These signals arrive in sequence, as a butterfly effect.
The first movement appears in policy and reimbursement guidance.
As CMS releases proposed rules, HCPCS applications, and payment threshold updates, Humbi allows teams to evaluate how those changes may reshape Medicare Part B and Part D economics based on historical utilization and reimbursement patterns.
From there, policy changes translate into care delivery behavior.
As economics shift, site-of-care decisions adjust. Administration begins migrating from hospital outpatient departments into physician offices and infusion centers. Humbi makes these movements visible as they start, often months before aggregate claims trends reflect meaningful displacement. These shifts are visible through site-of-care and utilization dashboards that break volume down across hospital outpatient departments, physician offices, infusion centers, and providers. This reveals where TRx is likely to follow the patient next.
Payer behavior then accelerates the shift.
Coverage criteria evolve, prior authorization logic tightens, and benefit designs are refined to align with emerging care settings. These changes rarely announce themselves through immediate denial spikes. They surface as quieter policy adjustments that indicate where access pressure will concentrate next. Integrated payer insights, built on payer landscape dashboards, payer attribute scoring, and payer mix analysis, reveal which plans are tightening access first and where TRx exposure is most concentrated. These views also support share-shift analysis and inform contracting impact discussions over the following quarters.
Taken together, these movements form a pattern. Policy sets direction. Care delivery responds to economics. Payer controls reinforce the outcome. Humbi’s actuarial intelligence connects these dots so access risk is visible early enough for teams to decide how and where to respond.
From Early Signal to Decisive Action
Early visibility only creates value if it changes decisions.
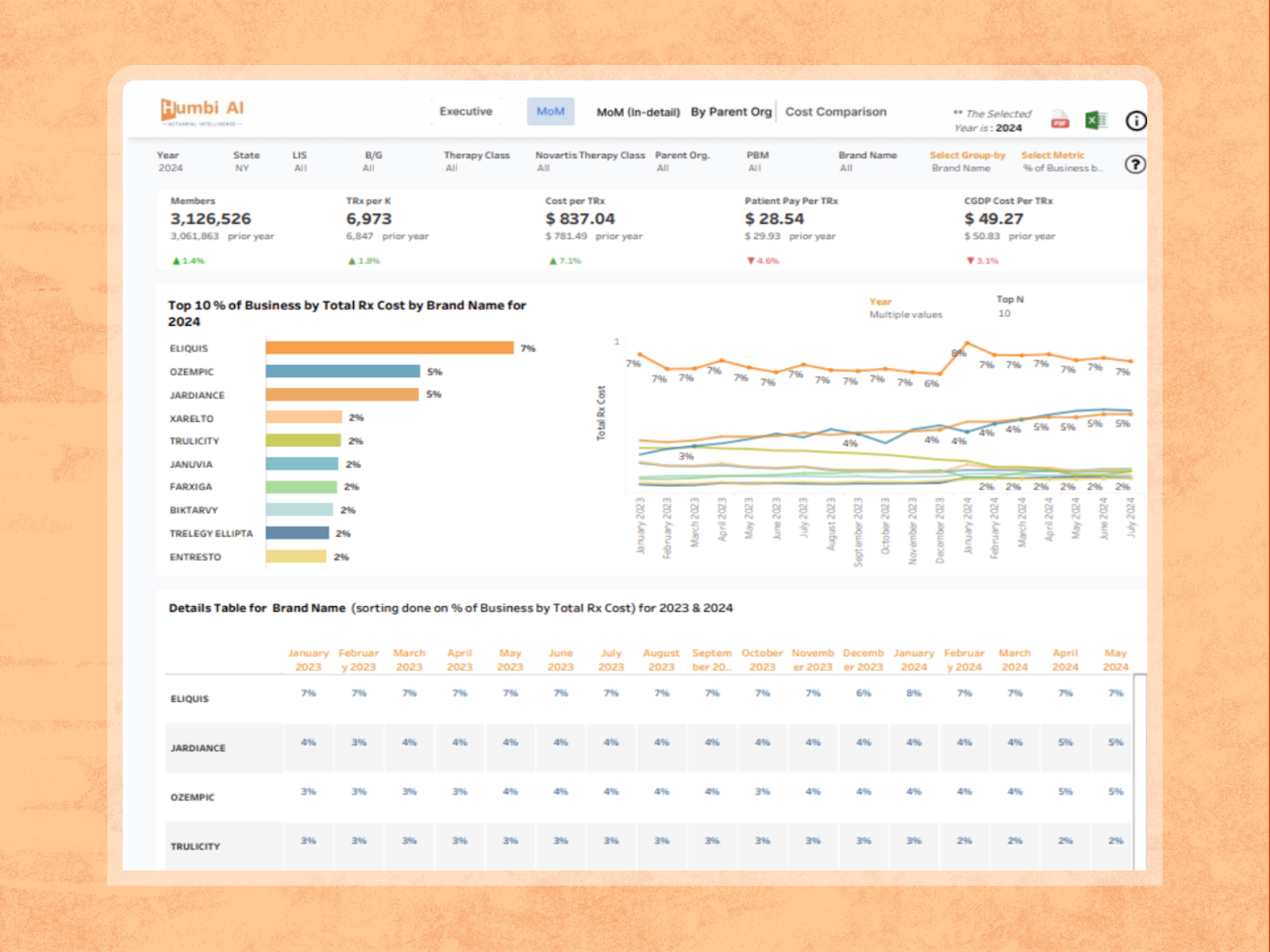
Humbi applies actuarial intelligence to contextualize them, helping your team separate material risk from background noise. Signals are evaluated based on population size, payer concentration, site-of-care sensitivity, and revenue exposure, so attention is focused where intervention can still protect TRx.
From there, early signals are translated into operational terms. Real-world utilization and payer mix inform expected TRx displacement, channel risk, and gross-to-net exposure. Instead of debating regulatory nuance in the abstract, your team can see the financial implications clearly enough to prioritize action.
That clarity enables faster, more precise responses. Contracts can be re-evaluated and reprioritized where site-of-care exposure is emerging. Field resources can be redirected toward payers showing early tightening. Patient support programs can be aligned before abandonment trends surface in claims.
Time becomes the compounding advantage. Acting even weeks earlier preserves volume that cannot be recovered once access pathways harden.
Why Actuarial Intelligence Changes the Experience
Traditional actuarial services are designed to validate outcomes after utilization stabilizes. That approach works for reporting, but it leaves a critical blind spot in fast-moving access environments.
Humbi closes that gap by combining comprehensive, patient-level claims data with actuarial intelligence that interprets early movement, not just final outcomes. Within Humbi, actuarial intelligence means applying actuarial methods such as risk adjustment, cohort normalization, utilization benchmarking, and financial modeling, directly to real-world claims data. Instead of treating policy changes, utilization shifts, and payer behavior as isolated signals, Humbi connects them into a quantified access risk view that market access teams can evaluate, prioritize, and act on.
The result is earlier clarity, grounded in comprehensive Medicare, Medicaid, and commercial data, and delivered through analytics designed specifically for market access, HEOR, and commercial strategy teams.
For teams navigating Medicare drug price negotiation and preparing market access strategy for 2026, this shift is decisive. You move from reacting to payer moves to anticipating them, from explaining lost volume to preventing it.
The Decisive Question
The question is not whether coding changes and site-of-care leakage will affect your products. The question is whether you'll detect them when you can still protect your market position.
If you're ready to move from retrospective validation to proactive intelligence, the next step is understanding how Humbi's actuarial intelligence platform integrates with your current workflows, data environment, and market access priorities.
Schedule a demo with our experts to explore how early access signal detection fits within your strategy.
Humbi by Innovaccer is an actuarial intelligence platform enabling life sciences organizations to manage risk, improve performance, and succeed in value-based care through comprehensive data access, advanced analytics, and actuarial expertise.



